Grow your practice. Brand your services and clinic. Become an Osteopractor.
The Diploma in Osteopractic is an intensive 12 to 18-month post-graduate training program that is awarded to licensed physical therapists or medical physicians that have successfully completed all of the following curriculum:
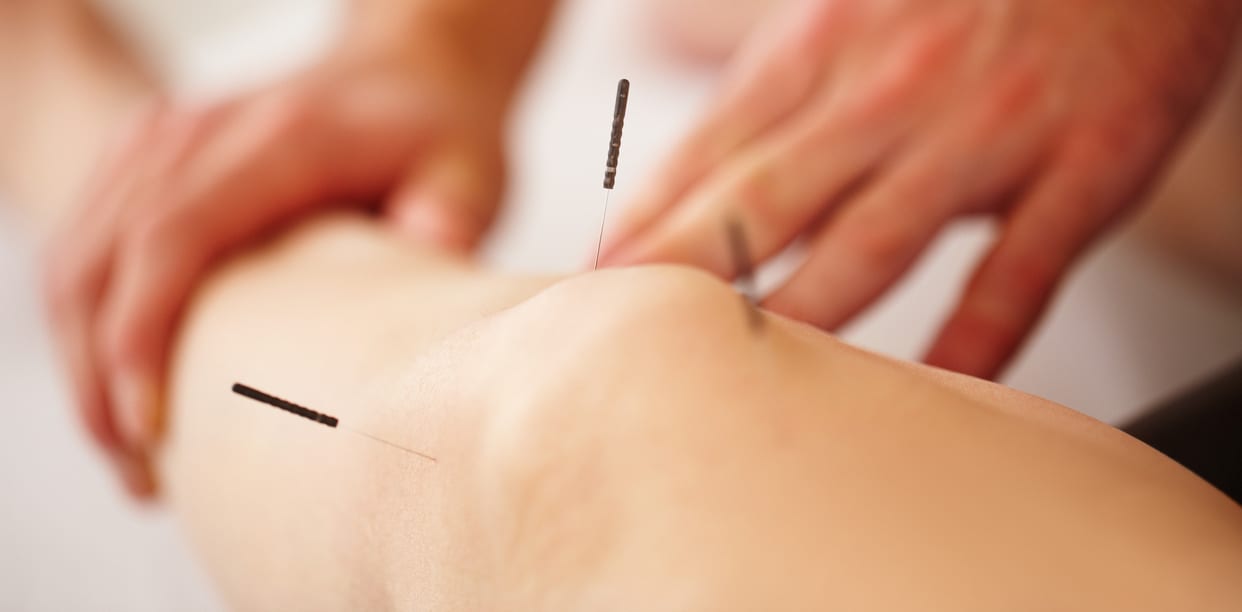
- Certified in Dry Needling (Cert. DN) by completing the DN-1 and DN-2 dry needling courses
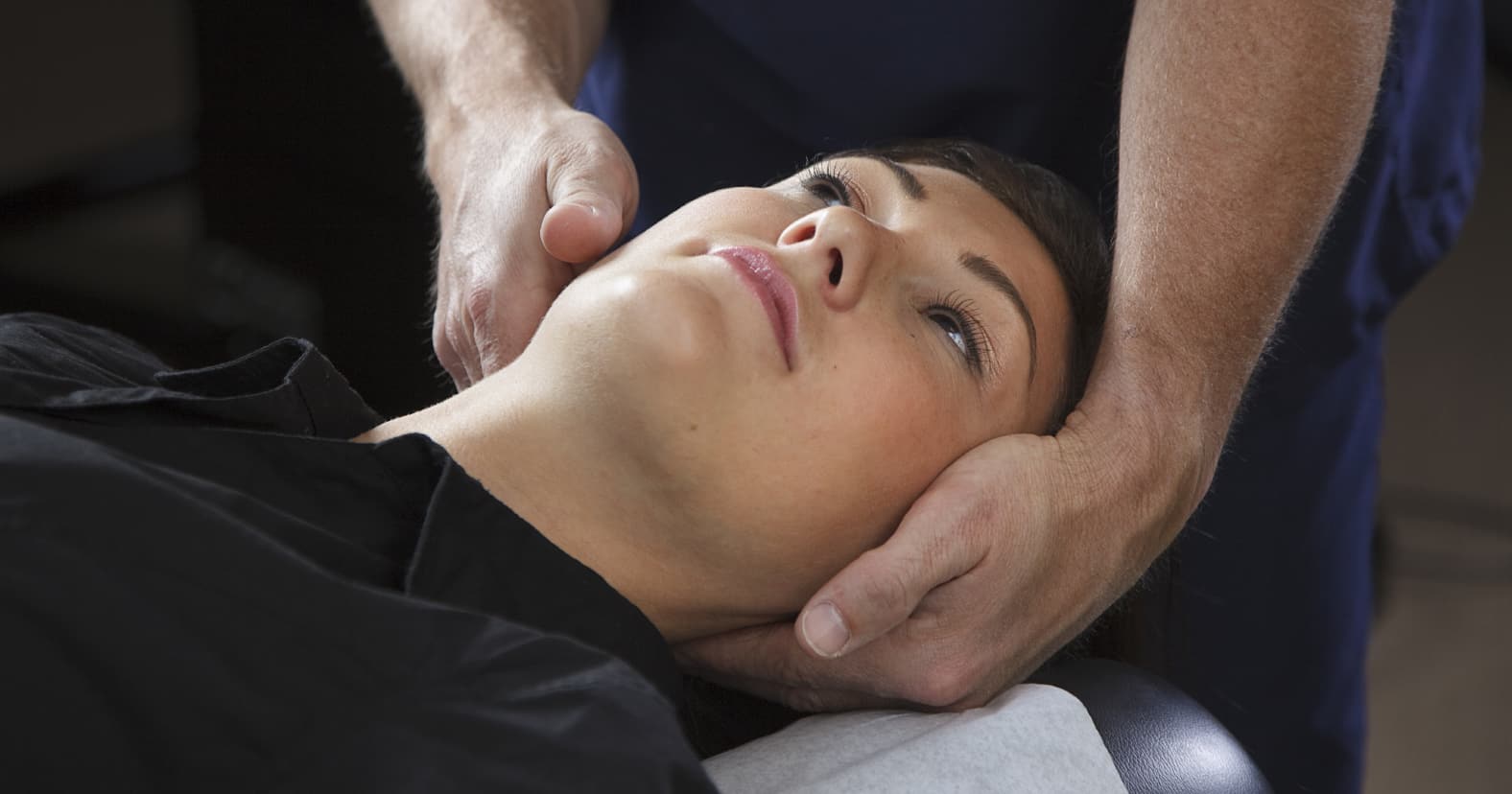
- Certified in Spinal Manipulative Therapy (Cert. SMT) by completing the osteopractic HVLA thrust spinal manipulation series
- Extremity Manipulative Therapy (EMT-1) in osteopractic HVLA thrust manipulation of the upper and lower extremities course
- Certified Vestibular Concussion Specialist (Cert. VCS) for differential diagnosis & management of sports-related concussions and high/low level patients with dizziness disorders
- Differential Diagnosis & Multi-Modal Management (DD-1) of upper & lower extremity spine related pain syndromes course
- Ultrasound-Guided Dry Needling (DN-3) with diagnosis & management implications for spine & extremity musculoskeletal conditions course
While the course work typically requires a minimum of 12 to 18 months to complete, the requirements for the Diploma in Osteopractic may be completed over a longer period.


An Osteopractor is a physical therapist, medical doctor, or doctor of osteopathic medicine that has completed an evidence-based post-graduate training program in the use of spinal and extremity thrust manipulation, ultrasound-guided dry needling, instrument-assisted manual therapies, and differential diagnostics for the diagnosis and treatment of neuromusculoskeletal conditions.
Osteopractic Physical Therapy is an approach to care, a sub-specialty within physical therapy, and more accurately describes the kind of physical therapy services (rather than simply “physical therapy”) offered so the public, potential patients and colleagues alike, can identify the appropriate practitioner of choice for the condition in question.
When you break a bone, you look for an orthopedist, not just a general medical doctor. When you have a skin condition, you go to the dermatologist. When your child needs medical care, you look for a pediatrician, not just a general medical doctor. Likewise, when you have neck pain, low back pain, headaches, tennis elbow, heel pain, carpal tunnel syndrome, knee osteoarthritis, plantar fasciitis, shoulder impingement, or joint pain etc., it makes sense to look for a specialist within physical therapy, i.e. an Osteopractic Physical Therapist or Osteopractor, not a generalist, that is specifically trained and has advanced post-graduate qualifications to treat neuromusculoskeletal conditions.
Osteo- orginates from the Greek osteon (“bone”) and –practor orginates from the Greek praktikos (“to practice, do, or perform”). Although the term osteopractor literally translates to “bone practitioner”, the most recent evidence-based practice guidelines for musculoskeletal disorders clearly supports a “multi-modal” approach; therefore, in addition to the joints (i.e. the bones), the direct treatment of myofascial trigger points, tendons, ligaments and fascia (all connected to the bones…) is certainly recognized within the osteopractic approach for optimal patient management. Likewise, a neurosurgeon doesn’t just operate on nerves during surgery, and osteopaths don’t just treat bone diseases.
The term osteopractor has nothing to do with the chiropractic or osteopathic professions; that is, the osteopractic concept is firmly focused on the management of neuromusculoskeletal disorders in an evidence-based fashion, not the treatment of other organ systems as the profession of chiropractic has traditionally engaged. More specifically, Osteopractors do not subscribe to the theory of the “Vertebral Subluxation Complex” as the primary cause of “dis-ease”. In short, Osteopractic Physical Therapists do not diagnose or treat all 10-organ systems as chiropractors are trained and licensed to do, and they do not utilize medicine or surgery as osteopathic physicians are trained and licensed to do. Lastly, spinal manipulation and dry needling are shared procedures between many healthcare professions (i.e. no one profession owns these procedures, e.g. 2012 Supreme Court Ruling: Alabama State Board of Chiropractic vs. James Dunning); however, the philosophy, the clinical reasoning, and the conditions treated with these procedures dramatically differs between professions.
We teach the scientific principles and the specific hands-on-skills necessary to achieve safe and effective thrust manipulation of the cervical, thoracic, lumbar, sacroiliac, and rib articulations. Furthermore, we teach how to safely deliver very specific and highly effective thrust manipulations to the upper cervical atlanto-axial (C1-2) and occipito-atlantal (C0-1) joints and the “difficult to get” first and second rib articulations.
Spinal Manipulation Institute teaches course attendees how to gain mastery over those difficult to manipulate junctional zones including the craniocervical, cervicothoracic, thoracolumbar and lumbosacral regions. We teach the specific psychomotor skills necessary to become a specialist in spinal manipulative therapy.
Have you ever wondered what the audible “cracking” sound really is? What is the average number of “pops” that should occur from a successful cervical manipulation? Is the “pop” or cavitation necessary to elicit the neurophysiological reflexive muscular relaxation of, for example, the scalenes or piriformis muscles? How much pre-load force do I need before I thrust the joint, and is this different in different spinal regions? How much peak force do I need to achieve successful manipulation in the upper cervical spine?
How fast do I need to be? Will more thrust speed reduce the peak forces needed to achieve cavitation of the target joint? That is, how high is the “high-velocity” in thrust manipulation of the spine? Is the acceleration of the thrust important? How long do I thrust for? Or what is the mean duration of a high-velocity low-amplitude thrust manipulation? Do the vertebrae actually move or change position when I manipulate them, is there evidence for this? How much pre-manipulation rotation, translation, and lateral flexion do I need?
Should I be pricking just muscular trigger points one at time or using needle rotation and leaving multiple needles in place for 20-30 minutes? Can I use dry needling to treat enthesopathy in the case of lateral epicondylalgia or Achilles tendinosis, i.e. attachment dysfunction of ligament or tendon against bone? Is there evidence to support the use of periosteal electrical dry needling for knee osteoarthritis or plantar fasciitis? These are some of the questions that will be answered when you take a course from Dry Needling Institute. Dry needling is certainly much more than pricking muscles one at a time!
We will demystify spinal manipulation and dry needling for you. All of the above are technicalities, we know. However, on a Spinal Manipulation Institute two-day course, or a Dry Needling Institute three-day course, we strive to take you from where ever you are, integrate your existing knowledge with ours, fill in the gaps, and enable you to master the art and science of spinal manipulation and dry needling.
No prerequisites are required. That is, we are committed to teaching all licensed practitioners (PT, DO, MD) without having them first spend a lot of time and money on prerequisite courses that are not necessary or completely relevant to learning the art and science of spinal manipulation. In fact, we believe learning how to perform a muscle energy technique or perform a C5-6 grade IV mobilization does not augment the practitioner’s propositional, procedural or tacit knowledge required to become a master at spinal manipulation. Why spend years learning softball if your goal is to play baseball? Furthermore, we think you have the knowledge base and learning abilities by virtue of your professional license; this is why we allow you to take our courses in spinal manipulation without any prerequisite courses.